Although breast augmentation is the most common plastic surgery operation in the world, the procedure is not without risks. Far and away the most common and feared risk for any patient considering getting breast implants is capsular contracture. The complication arises from scar tissue formed around breast implants that can cause breasts to harden, look and feel abnormal, and even potentially cause pain.
In the early days of breast augmentation surgery, capsular contracture rates were extremely high – 50% and above. Today, thanks to a growing pool of research and new surgical techniques, a well-informed breast surgeon can bring the risk to potentially less than 2%. Dr. William P. Adams Jr. of Dallas, TX discusses capsular contracture and the best ways to prevent it from happening.
What Is Capsular Contracture
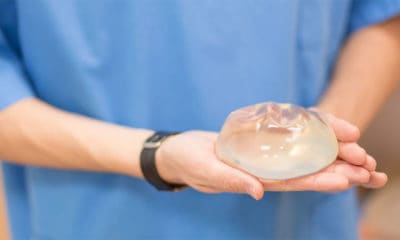
“Capsular contracture is a scar or tightening of the membrane that goes around the breast implant,” explains Dr. Adams. Basically, it’s the immune system’s response to a foreign material in the body. Whether it’s a pace maker, an artificial joint, or a breast implant, the body’s natural response is to form a protective membrane or shell, called a capsule, around the object.
The progression of capsular contracture when concerning breast implants is as follows:
- The breast feels a little firm, but appears normal.
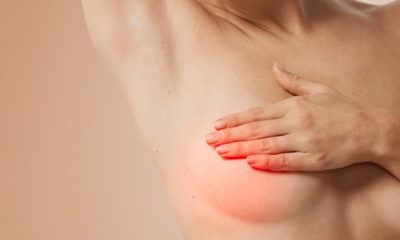
- The breast feels firm and appears abnormal.
- The breast feels hard, is painful to the touch, and appears abnormal.
Causes & Cures
For decades, capsular contracture has been the single greatest risk in both aesthetic and reconstructive breast surgery. There have been any number of theories as to what causes it, many of which have been proven false, but the one thing that we know for certain contributes more than any other to an increased risk of capsular contracture, “is colonization of bacteria around the implant,” explains Dr. Adams.
The bacteria causes chronic inflammation which results in the thickening or tightening of the capsule around the implant. To solve this issue, surgeons have implemented preemptive techniques to hopefully avoid the complication altogether, instead of correct it after the fact. The main technique is to be as thorough as possible in reducing the amount of potential contaminates during the operation so no bacteria finds it’s way onto the implants.
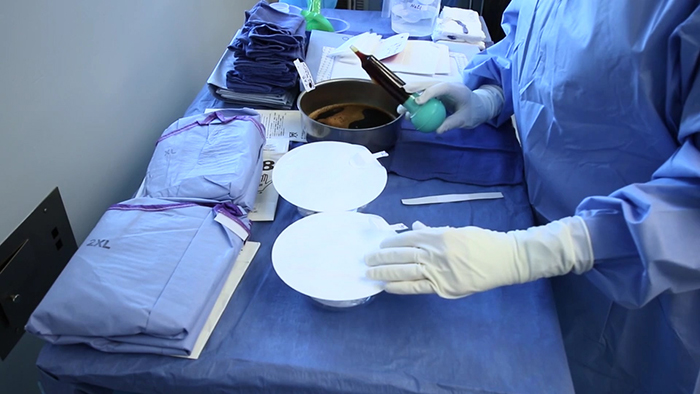
There’s always bacteria present during surgery; it’s a fact of life. The goal is to reduce the number of bacteria by following steps that include limiting bleeding, minimizing dissection in the breast tissue, covering the nipples in plastic during surgery, choosing the infra-mammary approach to insert the implant, and using antibiotic irrigation to wash out the pocket and minimize skin contamination. Following a collection of these steps has been shown to reduce capsular contracture rates by a level of 10.
While most patients who are going to get capsular contracture will do so within the first year, some patients don’t get it until they’ve had their implants for 8 or more years. There are no guarantees. The best way to avoid it is to see a surgeon who routinely performs breast augmentation surgery. An experienced breast surgeon will be up-to-date with all of the latest science and techniques to avoid breast augmentation complications and will have plenty of time in the OR to see a variety of unique situations.
By speaking with your surgeon about the potential complication and their experience in preventative surgical techniques, Dr. Adams feels that, “you can really minimize the risk of the patient developing capsular contracture.”
VIDEO TRANSCRIPT
ADAMS: Capsular contracture is a scar, or a tiny little membrane, that goes around the breast implant. When you put in any kind of implant, whether it’s a breast implant, or a pacemaker, or any kind of surgical implant, the body forms a membrane around them called a capsule.
ADAMS: Usually in a breast implant that’s not detectable – we don’t even know it’s there. But if it tightens around the implant, it can make the breast look misshapen. It can feel firm to the touch.
ADAMS: The number one cause is really colonization of bacteria around the implant that causes inflammation chronically and a response of that membrane or capsule to thicken and tighten around an implant.
ADAMS: What we have found is that there is a significant impact of capsular contracture based on surgical technique. And that includes mainly reducing the amount of contaminates or bacteria that can end up around the implant. Because the less bacteria the less chance that you can have a problem or a development of capsular contracture.
ADAMS: We actually just published a paper on this. We call it the 14 point plan. There’s 14 steps that we can take intraoperatively to reduce the risk of capsular contracture by reducing the amount of bacteria around the implant.















William P. Adams, Jr., MD
January 10, 2017 at 10:04 am
Dan
Breast augmentation revision with removal of the capsule and replacement is the typical treatment. When performed with all the steps of what we call the 14 point plan including special antibiotic irrigations the results are excellent.
Dan Voltz
January 10, 2017 at 9:56 am
I know capsular contracture may not be the most exciting topic, but this article is great! Can a breast augmentation revision procedure be used to help the patient get desired results after a contracture? Or do the implants have to come out due to the scar tissue (with no replacement possible)?