After finally deciding to take the plunge and schedule a breast augmentation, the decision-making process truly begins. One of the most important of the decisions patients will make is to choose from the modern incision options. There are countless articles and forums explaining why which is better – or worse – than each other, which can be helpful for patients looking for more information. The only potential downside of access to information is the potential for discovering poor and misguided information.
Board certified plastic surgeon Dr. Mark Epstein of Stony Brook, NY helps break down some of the myths on breast implant incisions and walks through the four most common options.
Four Breast Augmentation Incision Options
There are a myriad of decisions that you will need to make when it comes to your breast augmentation. While breast implant type, size and shape often get the most press, the one that really seems to trip up a lot of patients is the incision. Generally there are common four options:
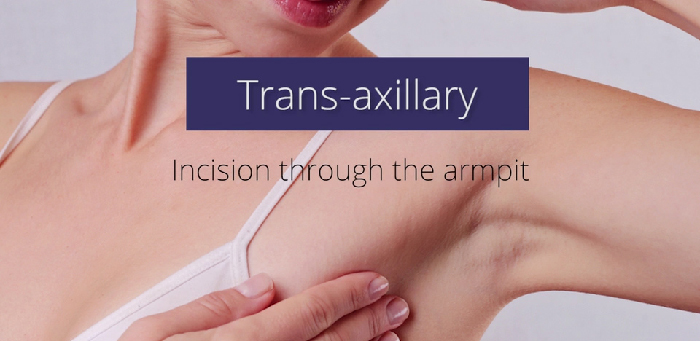
- the trans-axillary approach where the incision is placed in the arm pit
- the periareolar approach where the incision is placed around the areola
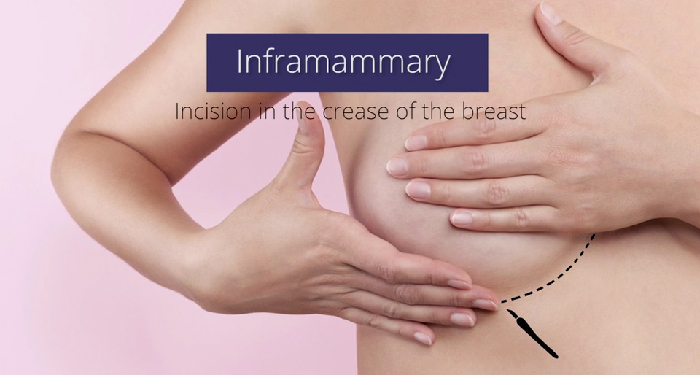
- the inframammary approach where the incision is placed under the breast in the fold
- the trans-umbilical approach where the incision is placed in the belly button
The problem for any surgical patient is the scar. While it is the trade off for an improved appearance, most patients are terrified of a visible, ugly scar, especially on the breasts. This can cause many breast augmentation patients to become enamored with the trans-axillary or trans-umbilical approach because they think that the scar will be hidden without really understanding the pros and cons.
The trans-umbilical approach only works with a saline implant. The surgeon makes a very small incision in the belly button through which he places a rolled up, deflated saline implant. The incision is too small for a silicone gel implant to pass through, which is one of the main drawbacks of this type of incision.
The trans-axillary approach through the arm pit also works very well with a saline implant. However, with a silicone implant, you will need an incision that is big enough for the surgeon to place the implant without damaging or weakening it. Epstein’s concern is, “that you’re going to need an incision that’s so long that you’re kind of defeating the purpose of a hidden incision.”
The periareolar approach works with both saline and silicone implants. It also allows the surgeon to do a dual-plane pocket. However, the surgeon needs to go around the nipple, exposing the ducts with bacteria in it which surgeons believe increases the chance of capsular contracture. The other problem that Dr. Epstein has with this approach is that he has to cut directly through the breast tissue in order to get access to the underside of the breast or the muscle and, “that causes a lot of internal scarring and damage to the breast even though you don’t see it from the outside.” This further increases a patient’s risk of capsular contracture. Also, the scar here is not always as invisible as people think, and if it is visible, “it’s on the most visible portion of the breast.”
The Inframammary Incision
“My favorite approach is to go under the breast, in the crease,” explains Dr. Epstein. While any scar is going to be slightly visible, the scar under the breast is hidden by the natural fall of your breast tissue. Furthermore, when the surgeon goes under the breast, he or she has much greater access to do what needs to be done to create a dual plane pocket, and release the pectoralis muscle. This gives the surgeon much more precision. It also works equally well with either a saline or silicone implant.
For Dr. Epstein, the inframammary approach results in, “a lot less downtime and a lot less bleeding because there’s no need for any blunt dissection.” With any breast augmentation, you want, “the least amount of exposure to bacteria and the least amount of trauma to the breast tissue” because this will not only greatly reduce your risk of capsular contracture, but will result in the easiest recovery and the lowest chance of needing revision surgery in the future.
“Having tried several different options, at this point in my practice, I prefer the imframammary approach,” explains Epstein. “It gives the greatest degree of control, the least amount of bleeding, the greatest flexibility to create the pocket the way that I want it, the least visible a scar and overall, I get the best cosmetic result.”















Facebook
Twitter
Instagram
YouTube
RSS