Labiaplasty is experiencing a dramatic rise in popularity over the last 5 years. Second only to buttock augmentation in growth, the number of labiaplasty procedures has jumped 52.9% since 2014 – a remarkable figure. The significance of it’s rise is more or less related to the fact that women just didn’t know it was an option. Not only that, they also didn’t know that the procedure affects more than just aesthetics, but function, too.
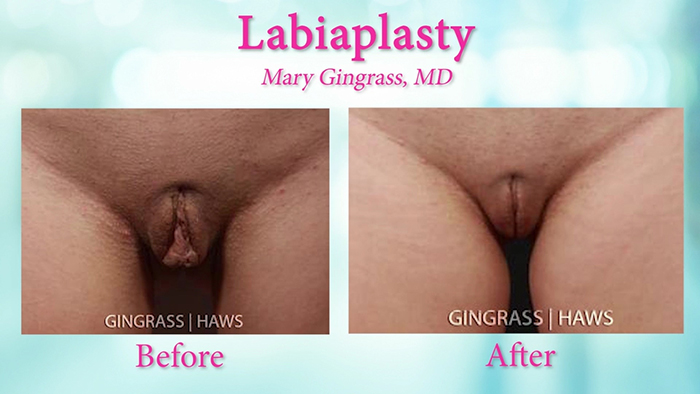
Labiaplasty is a procedure aimed at altering the labia minora and/or labia majora, or the folds of skin surrounding the vulva. Generally, the procedure looks to aesthetically improve the area by trimming excess skin and tissue, but it can provide significant functional improvement as well for women in their middling years. Issues such as urinary stress incontinence and an excessive labia minora causing discomfort during physical activity are a number of reasons why women are seeking the procedure. In many of these cases, the aesthetic improvement is icing on the cake to the real benefit they received by solving long-standing issues of discomfort and aging. Better yet, labiaplasty is a fairly “simple” procedure that can be done swiftly and efficiently.
Due to the success of labiaplasty, more and more women have realized the potential benefit it may provide. Many of these women may have never participated in plastic surgery before, and therefore are worried about elective surgical procedures and the risks associated with general anesthesia. Because a labiaplasty procedure generally is short, one of the most asked questions is whether or not it can be performed in an office setting under local anesthesia. Board certified plastic surgeon and expert on labiaplasty, Dr. Mary Gingrass of Nashville, answers this question in the latest PSC FAQ.












Facebook
Twitter
Instagram
YouTube
RSS